What to Expect
We make every effort to create an environment that is safe, supportive, and caring for all of our patients through clinical excellence and trauma-informed, patient-centered care. Our team is committed to hearing each client's story and understanding their concerns to be able to create an individualized and specific health care plan.
All evaluations and treatments are completed one-on-one in a private room with a pelvic health therapist. Each visit will include hands-on external and internal exams depending on the client’s comfort level.
Included Treatments
Strengthening Exercises
Hands-on training with exercises aimed at strengthening the pelvic floor and inner core muscles. This is essential to properly to support your organs, for sexual function, and stability.
Relaxation Techniques
We provide training with specific stretches and calming techniques to provide awareness and full release of the pelvic floor muscles.
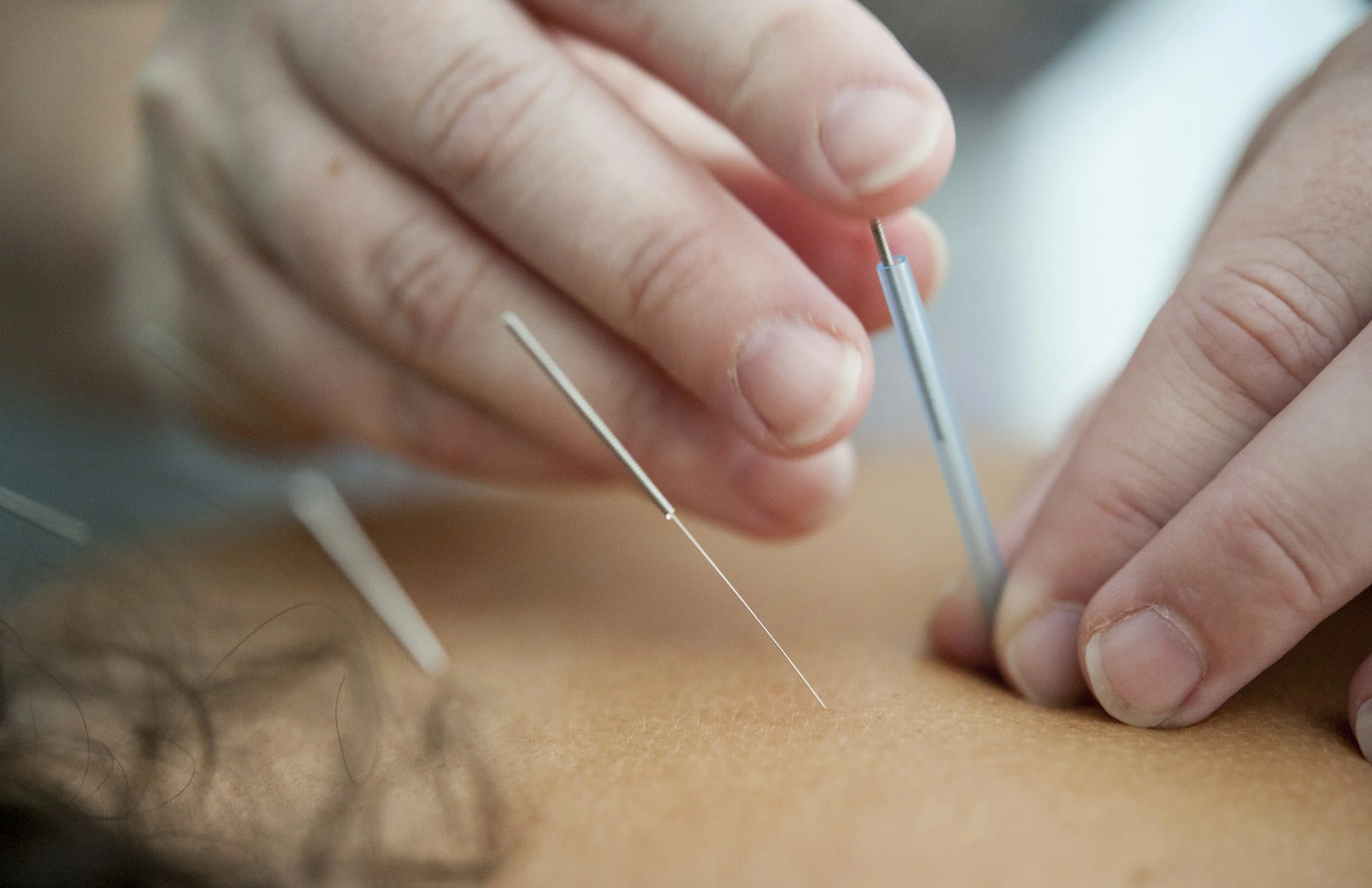
Dry
Needling
Treatments for musculoskeletal pain and movement impairments can include using thin, filiform needles through the skin into myofascial trigger points (i.e., tight "knots" in a muscle) that can cause pain and restricted motion.
Manual Therapy
We are muscle specialists! Myofascial release, dry needling, trigger point release, and massage are vital to tissue healing both internally and externally. This allows the muscles to stretch and relax for full function and pain-free motion.
Frequently Asked Questions
-
If you’re experiencing bladder, bowel,pain, or sexual health concerns, there’s a good chance we can help.
At Wonder Pelvic Therapy & Wellness, we specialize in pelvic health and whole-body care. We treat symptoms involving the pelvis, hips, abdomen, and tailbone—essentially the region from your waist to your upper thighs.
This may include:
leakage
constipation
pelvic pressure
tailbone pain
difficulty returning to exercise
If you’re unsure whether pelvic physical therapy is right for you, we’re happy to talk it through and help you take the next step.
-
We are the only clinic in the High Country solely dedicated to pelvic health.
What makes us different:
Specialized training in pelvic health
60-minute, one-on-one sessions with your licensed physical therapist
No double-booking
No passing you off to aides or techs
Calm, private treatment rooms
Whole-person approach (nervous system, movement, strength, lifestyle)
Individualized care tailored to your specific needs
Longer visits designed for depth and connection
Not limited by insurance-driven visit caps or treatment restrictions
-
At your first visit, you will meet in a private treatment room with one of our physical therapists. The therapist will ask questions related to:
your pelvic health history,
symptoms, and
goals to fully understand your concerns.
Your evaluation may include looking at movement, strength, coordination, and how your body manages pressure. In some cases, a pelvic floor muscle assessment may be helpful to better understand your symptoms. This is always discussed beforehand and only performed with your consent — and it is not required for care.
We encourage questions throughout your visit and will explain everything along the way. Your treatment plan will be individualized and evolve with you at each session. Call us today if we can answer any additional questions about your first visit.
-
Making a decision to put your health first is one of the most important steps in preparing for your first appointment.
Helpful Strategies:
Having a generalized timeline of how and when your symptoms began is very helpful,
A list of your personal questions you’ve written before coming to physical therapy.
We want to make sure we address your concerns and needs during each session and appreciate as much information as you can share with us.
-
Yes.
While many of our clients are women, we work with individuals of all genders experiencing pelvic floor dysfunction, bowel or bladder concerns, pelvic pain, core weakness, or return-to-activity goals.
Pelvic health is not gender-specific — and everyone deserves specialized, respectful care. You can explore all of our services to find answers related to your symptoms.
-
Patients have direct access to physical therapy in the state of North Carolina, meaning that a referral from a medical provider is not required to initiate therapy.
Some insurance companies may require a physician referral for reimbursement. If you are pregnant, a referral is required to ensure you and the baby are medically stable prior to treatment.
-
Pelvic physical therapy isn’t only for when something feels wrong.
Many people come to us proactively — to prepare for pregnancy or birth, return to running, improve strength and performance, or simply understand their pelvic floor and core better.
We can assess movement, coordination, pressure management, and strength to help you prevent issues before they start and build confidence in your body.
Prevention and education are just as valuable as treatment. Call us today if you have additional questions related to your personal wellness needs.
-
You can begin pelvic physical therapy as soon as you feel ready—even within the first few weeks postpartum.
Early visits focus on education, breathing, gentle core connection, posture, scar support (including C-section), and guidance for bowel, bladder, or pain concerns.
If a pelvic floor muscle assessment is needed, we typically wait until about 4–6 weeks postpartum and after medical clearance. Internal assessment is not required to begin care.
You can find more information on postpartum care. Early support can help you heal more comfortably and confidently.